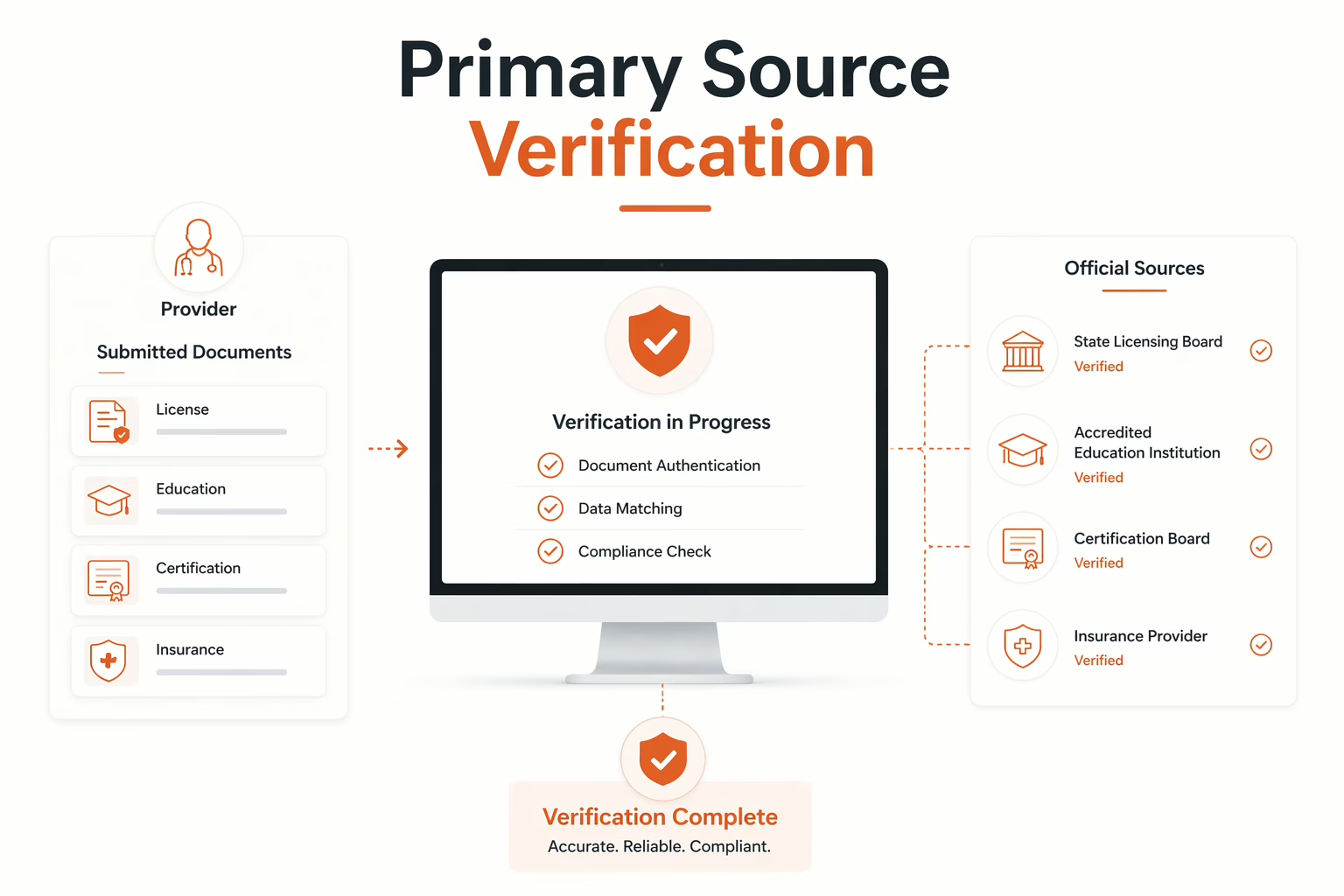
Primary source verification in credentialing is the foundation of safe, compliant, and reliable healthcare operations. For practice managers and healthcare administrators, primary source verification in credentialing ensures that every provider meets strict regulatory and quality standards.
In today’s environment, where compliance and patient safety are under constant scrutiny, relying on unverified information is a major risk. PSV is not optional—it is essential for protecting your practice, your patients, and your revenue cycle.
What Is Primary Source Verification
Primary Source Verification (PSV) is the process of confirming provider credentials directly from the original issuing source. This includes verifying education, licenses, certifications, training, and work history with institutions such as universities, licensing boards, and certification bodies.
Unlike secondary verification, PSV eliminates assumptions and ensures data accuracy at the source level.
Why Primary Source Verification in Credentialing Matters
PSV plays a critical role in healthcare credentialing and provider enrollment. Without proper verification, practices risk onboarding unqualified providers, which can lead to compliance violations, claim denials, and serious patient safety concerns.
1. Ensures Authenticity of Provider Credentials
PSV confirms that all submitted information is accurate and valid. This prevents reliance on outdated, incomplete, or falsified data.
2. Protects Patient Safety
Verifying credentials ensures providers are qualified to deliver care. This reduces the risk of medical errors and improves patient outcomes.
3. Maintains Healthcare Compliance
Organizations must comply with standards set by NCQA, CMS, and The Joint Commission. PSV ensures your practice meets these requirements and avoids penalties.
To strengthen compliance, it’s important to understand how credentialing processes work and why accuracy matters.
4. Prevents Fraud and Misrepresentation
PSV detects discrepancies in applications, such as expired licenses or false certifications. This protects your organization from fraud-related risks.
5. Reduces Financial and Legal Risk
Credentialing errors can lead to denied claims, audits, or lawsuits. PSV minimizes these risks by ensuring accurate provider data.
Step-by-Step: How Primary Source Verification Works
1. Collect Provider Information
Gather all credentialing documents, including licenses, certifications, and education records. Ensure information is complete before starting verification.
2. Identify Primary Sources
Determine the original issuing authorities for each credential. This may include licensing boards, universities, or certification organizations.
3. Verify Credentials Directly
Contact primary sources through official channels or databases. Confirm validity, status, and expiration dates of credentials.
4. Document Verification Results
Maintain clear records of verification, including dates and sources. Proper documentation is critical for audits and compliance.
5. Monitor and Re-Verify Regularly
Credentialing is ongoing, not a one-time process. Regular monitoring ensures providers remain compliant and qualified.
Impact on Revenue Cycle and Operations
Primary source verification in credentialing directly affects revenue cycle management. If credentials are not properly verified, providers may face delays in payer enrollment and insurance approval.
This prevents billing and leads to revenue loss. Accurate verification helps reduce payer delays, improve claim approvals, and maintain steady cash flow.
To avoid financial disruptions, practices should also focus on reducing payer enrollment delays and improving workflow efficiency.
Real-World Scenario: Preventing a Costly Mistake
Consider a clinic hiring a new specialist with impressive credentials. Without PSV, the provider is onboarded quickly and begins seeing patients.
Later, it is discovered that one certification had expired months ago. This results in claim denials, compliance issues, and potential legal exposure.
With PSV in place, this issue would have been identified before onboarding. This highlights how PSV protects both patient safety and financial stability.
Common Challenges in Primary Source Verification
Despite its importance, PSV can be complex and time-consuming. Practices often face delays due to slow responses from institutions or incomplete provider data.
Manual verification processes also increase the risk of errors and inconsistencies. Without proper systems, tracking expiration dates and re-verification can become overwhelming.
Best Practices to Improve PSV Efficiency
Standardize Credentialing Workflows
Create clear processes for document collection and verification. Consistency reduces errors and improves turnaround time.
Use Technology for Automation
Credentialing software can automate verification and tracking. This reduces manual workload and improves accuracy.
Maintain Centralized Provider Data
Keep all provider information in one system. This ensures consistency across credentialing and billing workflows.
Track Expiration Dates Proactively
Set reminders for license and certification renewals. This prevents lapses that could disrupt operations.
Train Staff on Compliance Requirements
Ensure your team understands regulatory standards and verification procedures. Well-trained staff reduce the risk of errors and delays.
Why Primary Source Verification Is Essential
Primary source verification in credentialing is the backbone of safe, compliant, and efficient healthcare operations. By implementing primary source verification in credentialing, practices can reduce risks, improve accuracy, and strengthen revenue cycle management.
Without PSV, practices face delays, compliance issues, and potential financial losses.
If your organization wants to streamline credentialing and ensure complete compliance, eClinicAssist is here to help. Our experts simplify verification, reduce administrative burden, and protect your practice from costly errors. Contact us today to get started with expert support.